про услугу
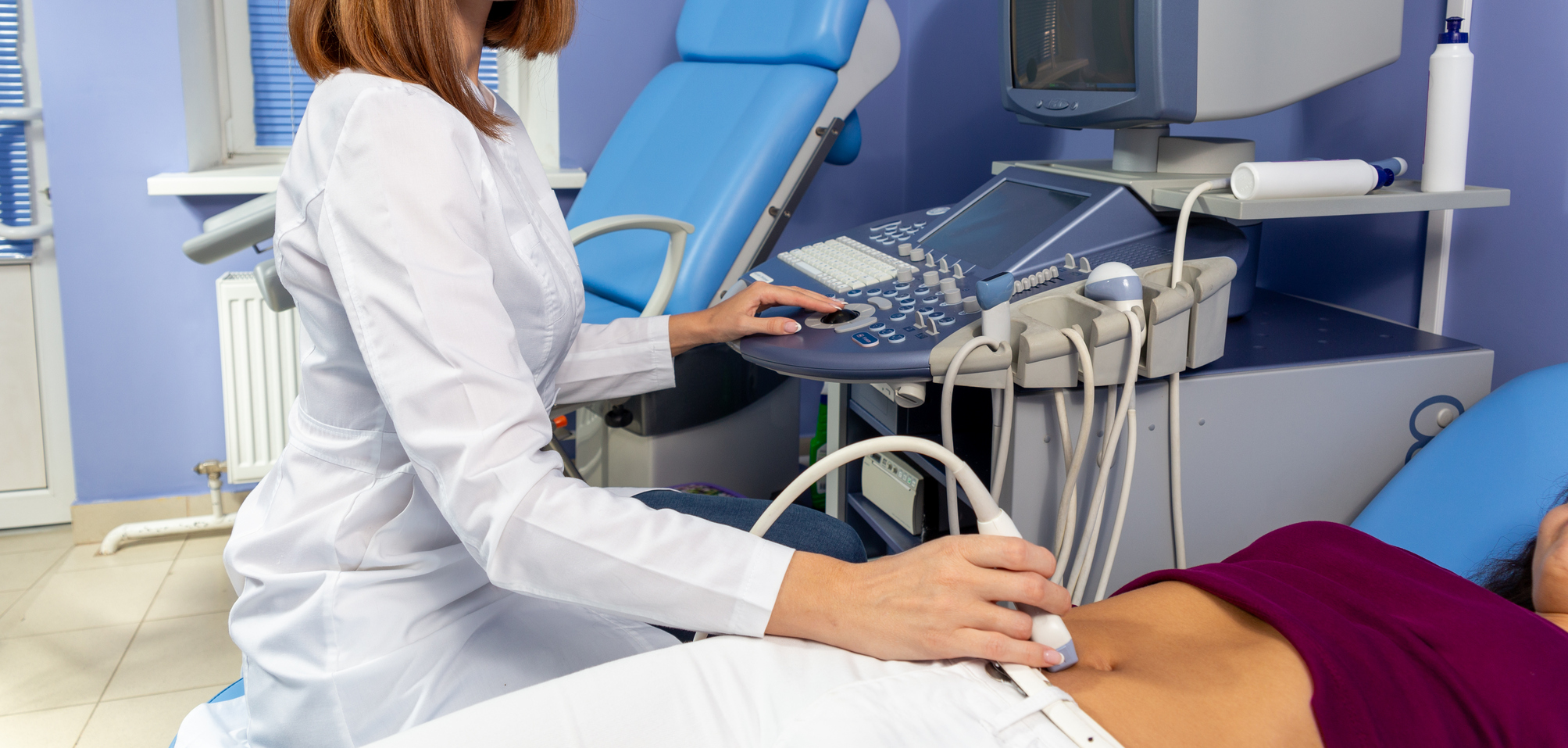
Суть и особенности процедуры
Манипуляция достаточно простая, чаще всего проходит без осложнений. По сути, это малоинвазивная гинекологическая манипуляция, во время которой производится забор тканей, необходимых для обнаружения аномалий.

Врач срезает или отщипывает небольшой участок с помощью иглы, скальпеля. Пункционная биопсия проводится под визуальным контролем при помощи кольпоскопа, гистероскопа. Полученный фрагмент направляется в лабораторию на гистологическое исследование.
Биопсия шейки матки — высокоточный и информативный способ диагностики женских болезней. Используется для диагностики различных заболеваний на ранней стадии развития. Позволяет дифференцировать онкологические заболевания, дисплазию, эрозию шейки матки и другие патологии. Процедура показана при подозрении на развитие злокачественных новообразований в области репродуктивных органов. Применяется для уточнения диагноза и определения тактики лечения. Предварительно проводится визуальный осмотр при помощи прибора кольпоскопа — оптического прибора с увеличительной линзой. При наличии показаний врач также может выполнить забор мазка из цервикального канала.
Взятый материал изучается под микроскопом. Это позволяет уточнить диагноз, подтвердить или исключить наличие ракового процесса, установить масштаб и степень поражения половых органов, составить план лечения.
Методы проведения исследования
Существует несколько способов проведения биопсии, выбор зависит от состояния пациентки.
-
Биопсия с кольпоскопией (самый популярный метод). Для взятия биоматериала применяется пункционная игла. Обезболивания не требуется. В первые три дня возможно небольшое кровотечение, которое обычно проходит самостоятельно.
-
Конхотомное исследование. Аналогично предыдущему методу с той разницей, что используется не игла, а хирургический инструмент, напоминающий кусачки или ножницы — конхотом. Манипуляция требует местной анестезии.
-
Радиоволновая методика. Малоинвазивная процедура, после которой не остается следов вмешательства, нет выделений из влагалища.
-
Использование лазера. Малотравматичный способ, однако он требует общего наркоза и наблюдения пациентки в стационаре.
-
Петлевой метод. Противопоказан при планировании беременности, так как после процедуры часто образуются рубцы на шейке матки. Также могут начаться длительные вагинальные выделения. Участок соскабливается при помощи электропетли под местной анестезией.
-
Круговая биопсия. Применяется с целью выявления и лечения патологий. Используется радиоволновой нож или скальпель. Процедура проводится под общим наркозом, требуется госпитализация женщины в стационар.
-
Эндоцервикальный кюретаж. Цервикальный канал выскабливается кюреткой. Необходимо местное обезболивание.
-
Клиновидный метод. Пока пациентка находится под общим наркозом образцы измененных тканей и прилегающих к ним участков иссекаются с применением скальпеля. Одновременно с ножевой биопсией гинеколог может провести выскабливание канала.
Среди различных тактик забора материала наименее травматичными являются прицельная биопсия с кольпоскопией и радиоволновой метод. При этих процедурах минимально повреждаются окружающие ткани, редко случаются осложнения, не происходит образования рубцов (в отличие от петлевой биопсии). При пункции могут возникать неприятные ощущения. Радиоволновая биопсия из-за безопасности и низкой травматичности рекомендуется при планировании беременности. А вот петлевая биопсия в этом случае противопоказана.
Когда нужно провести более детальное исследование, взять большой объем материала, проводится иссечение участка тканей конхотомом. Недостаток метода — в необходимости местной анестезии. Однако параллельно можно удалить полипы и кондиломы, что является преимуществом метода.
Эндоцервикальный кюретаж применяется очень редко, так как это достаточно болезненный метод, может привести к образованию спаек в канале шейки матки.
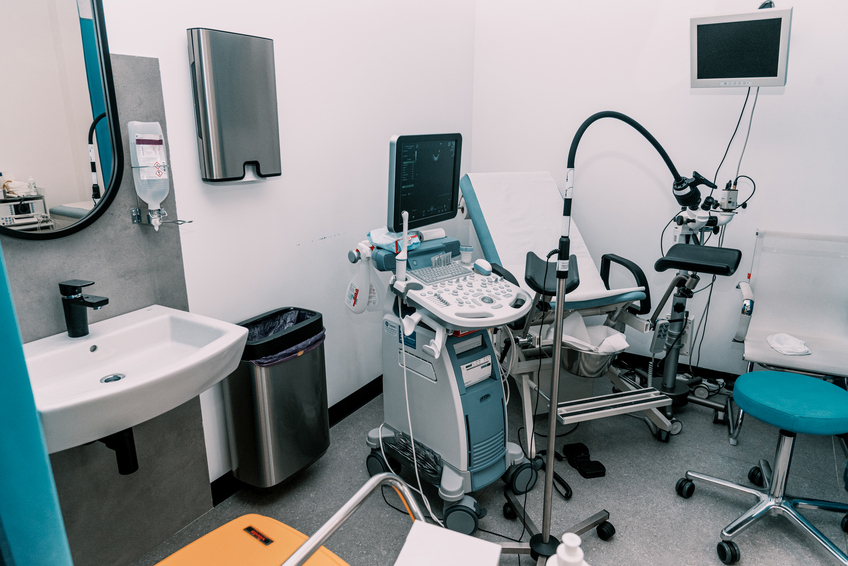
Взятие материала: показания
Процедура обязательна для женщин, имеющих генетическую предрасположенность к онкозаболеваниям половых органов. Обследование проводится, если при осмотре у гинеколога обнаруживаются подозрительные участки.
Врач назначает забор биоматериала, когда цитологическое исследование или кольпоскопия выявляют усиление сосудистого рисунка, неровность слизистой или другие патологические изменения.
Сдать биопсию шейки матки рекомендуется при наличии следующих патологий или подозрении на них:
-
злокачественные новообразования в области шейки матки;
-
предраковые состояния — лейкоплакия, дисплазия;
-
эктопия или эрозия шейки матки;
-
доброкачественные новообразования (полипы) в цервикальном канале;
-
рост половых бородавок — кондилом.
Биопсия шейки матки назначается только профильным специалистом при наличии объективных показаний к данной процедуре.
Противопоказания
Процедура связана с травмированием слизистой оболочки, поэтому имеется ряд ограничений. Анализ противопоказан в следующих случаях:
-
воспалительные процессы в репродуктивных органах;
-
инфекционные заболевания, передаваемые половым путем;
-
хронические болезни в стадии обострения;
-
менструация.
Важно серьезно подходить к подготовке к исследованию и вовремя выявлять противопоказания.
Как подготовиться к процедуре
Подготовка к биопсии шейки матки включает анализы и обследования, назначенные лечащим врачом. Это уменьшает риск осложнений.
Что включает предварительное обследование:
-
консультация, сбор анамнеза — врач уточняет жалобы пациентки, гинекологический анамнез, наличие сопутствующих заболеваний;
-
общий анализ крови и мочи;
-
коагулограмму;
-
гинекологический осмотр;
-
исследование с использованием кольпоскопа;
-
анализ на цитологию;
-
мазок на микрофлору;
-
анализы на папилломавирус, половые инфекции, гепатит, ВИЧ.
Доктор может назначить дополнительные обследования. Если имеются хронические заболевания, потребуется консультация соответствующих специалистов.
Самостоятельная подготовка включает ряд ограничений:
-
необходимо половое воздержание за несколько дней до биопсии;
-
накануне посещения клиники следует провести обычные гигиенические процедуры;
-
запрещается вводить в половые органы любые препараты, не назначенные доктором, в том числе не рекомендуется вводить тампоны, делать спринцевание.
Если забор тканей будет проводиться под общим наркозом, за 8 часов до его введения нельзя употреблять пищу.

Как проводится биопсия шейки матки: этапы и особенности
Процедура назначается врачом только после выявления признаков патологии по результатам предварительного обследования.
В зависимости от выбранного метода, биопсия может проводиться под общим обезболиванием или под местной анестезией. Часто применяется спинальное или эпидуральное обезболивание нижней части тела. Чтобы определить оптимальный вид обезболивания (если оно требуется) и подобрать сочетание препаратов, пациентку предварительно осматривает врач-анестезиолог.
Процедура выполняется в стерильных условиях врачом-гинекологом. В зависимости от выбранного метода она продолжается полчаса или дольше, в условиях стационара — до полутора часов.
С помощью скальпеля, пункционной иглы или другого инструмента производится иссечение тканей, осуществляется забор образца. Если начинается кровотечение, врач вводит тампон из марли (удаляется через пару часов).
Собранные образцы направляются в лабораторию на гистологическое исследование. Специалист-морфолог изучает клеточные структуры, строение эпителия и готовит подробное заключение.
Реабилитация
Продолжительность восстановления после биопсии зависит от вида процедуры и индивидуальных особенностей организма. При малоинвазивной процедуре заживление идет 7-10 дней, при более травматических и обширных - до нескольких недель. После окончания второй недели следует посетить гинеколога. Манипуляция малоинвазивная, не оставляет шрамов и рубцов, редко вызывает осложнения. Однако из-за риска инфицирования пациенткам следует контролировать свое состояние и самочувствие.
Возможные последствия после проведения биопсии шейки матки:
-
незначительное кровотечение;
-
тянущие боли в нижней части живота — снимаются обезболивающим.
Все это — нормальные реакции организма, которые не являются признаками осложнений, лечения не требуется.
К осложнениям относятся кровотечение из половых органов и инфицирование. Симптомы инфекции включают повышение температуры, неприятный запах выделений или выраженные боли внизу живота.
При появлении таких осложнений необходимо сразу же обратиться к доктору, который определит и устранит причину их появления.
Пациентка восстанавливается дома. Чтобы ускорить и облегчить реабилитацию, в течение 2 недель она должна соблюдать простые правила:
-
во время кровотечений, в том числе менструальных, не использовать тампоны, следует отдавать предпочтение гигиеническим прокладкам;
-
не делать спринцевание;
-
соблюдать половое воздержание (срок указывает врач);
-
мыться только под душем (не горячим);
-
не посещать сауну и баню;
-
избегать физических нагрузок, не поднимать тяжелые предметы.
Своевременная диагностика позволит выявить патологии шейки матки и их первопричины. Это сделает лечение максимально результативным, в некоторых случаях позволит применить щадящие методы, поможет избежать рецидивов. Пройти процедуру быстро, качественно, безопасно, без боли и осложнений вы можете в нашей клинике. Гинекологи Expert Clinics учитывают все имеющиеся показания и противопоказания, используют современное оборудование и передовые малоинвазивные методики. Это позволяет исключить дискомфорт и риски для пациентов. Сделать биопсию и пройти все подготовительные обследования можно в одном месте. Наши врачи сопроводят вас на всех этапах диагностики и лечения.
Вопрос/ответ
1) Сколько нужно лежать в больнице после биопсии шейки матки?
После окончания диагностической манипуляции женщина остается в стационаре минимум на пару часов, при необходимости — на один или два дня. Это необходимо для контроля за состоянием пациентки, предупреждения осложнений. Восстановление проходит в домашних условиях. При появлении тревожных симптомов следует обратиться к лечащему врачу, а также пройти осмотр через две недели после биопсии.
2) Какие заболевания может показать биопсия шейки матки?
Процедура позволяет диагностировать различные патологии шейки матки. Что показывает биопсия шейки матки:
-
предраковые состояния, включая дисплазию;
-
злокачественные или доброкачественные новообразования.
Обнаружение патологически измененных клеток позволяет своевременно начать терапию и предупредить развитие некоторых выявленных заболеваний.
Учтите, что только специалист может корректно расшифровать результаты исследования и подтвердить диагноз. Попытки сделать это самостоятельно приводят к ошибкам и нежелательным волнениям.
3) Что лучше: кольпоскопия или биопсия?
Оба метода применяются для ранней диагностики предраковых состояний, профилактики рака половых органов. Важно понимать: это два абсолютно разных метода диагностики и у каждого свои показания.
Кольпоскопия — визуальный осмотр влагалища, шейки матки, наружных половых органов, проводится с помощью специального устройства — кольпоскопа, который даёт многократное увеличение исследуемого участка. Биопсия — соскоб клеток эпителия для лабораторного анализа под микроскопом.
Осмотр с использованием кольпоскопа — безопасная процедура, не влияющая на вынашивание плода и возможность зачатия. А вот забор тканей может вызвать осложнения: кровотечение из влагалища, инфицирование. В период беременности биопсию проводят только в случае крайней необходимости.
Методики часто используются в комплексе. Биопсию назначают для уточнения результатов кольпоскопии и ПАП-теста при наличии показаний.