про услугу
Гинекологический мазок на флору — это стандартное исследование, которое помогает оценить состояние микрофлоры половых органов женщины и проводится практически при каждом визите к гинекологу.
Гинекологический мазок на флору — это стандартное исследование, которое помогает оценить состояние микрофлоры половых органов женщины и проводится практически при каждом визите к гинекологу.
Что это такое
Мазок на флору — это анализ, при котором берется биоматериал из слизистых оболочек половых органов (ПО) для определения их микробного состава. Основная цель — оценка состояния микрофлоры и выявление возможных отклонений, включая воспаление, инфекционные заболевания или дисбактериоз.
Под микрофлорой понимается совокупность микроорганизмов, обитающих на слизистой оболочке ПО. У здоровой женщины она представлена преимущественно лактобактериями (палочками Дедерлейна), которые обеспечивают защиту от патогенной флоры.
В лаборатории биоматериал исследуют под микроскопом, оценивая такие показатели, как:
-
количество плоского эпителия;
-
уровень лейкоцитов;
-
наличие патологических микроорганизмов (кокки и диплококки, споры или мицелий грибов, подвижные бактерии).
Показания для проведения анализа
Мазок на флору назначается в следующих ситуациях:
-
Профилактический осмотр, который подразумевает регулярную проверку состояния репродуктивной системы.
-
Подозрение на инфекции.
-
Боль внизу живота. В этом случае необходимо исключить воспалительные процессы.
-
Планирование беременности. На этом этапе важно оценить состояние микрофлоры перед зачатием.
-
После лечения инфекций для контроля эффективности терапии.
-
Перед операциями, для предупреждения инфекционных осложнений.
Рекомендуется сдавать его всем сексуально активным женщинам не реже одного раза в год.
Как берут мазок из половых органов
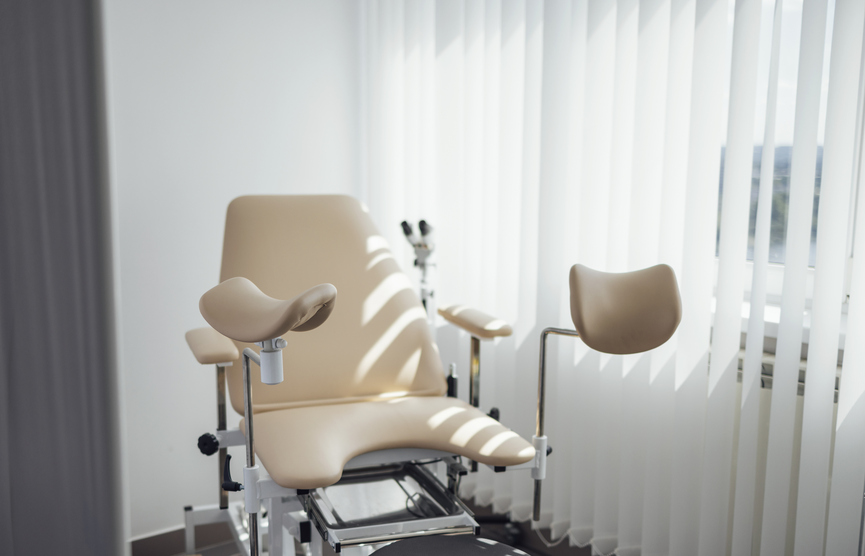
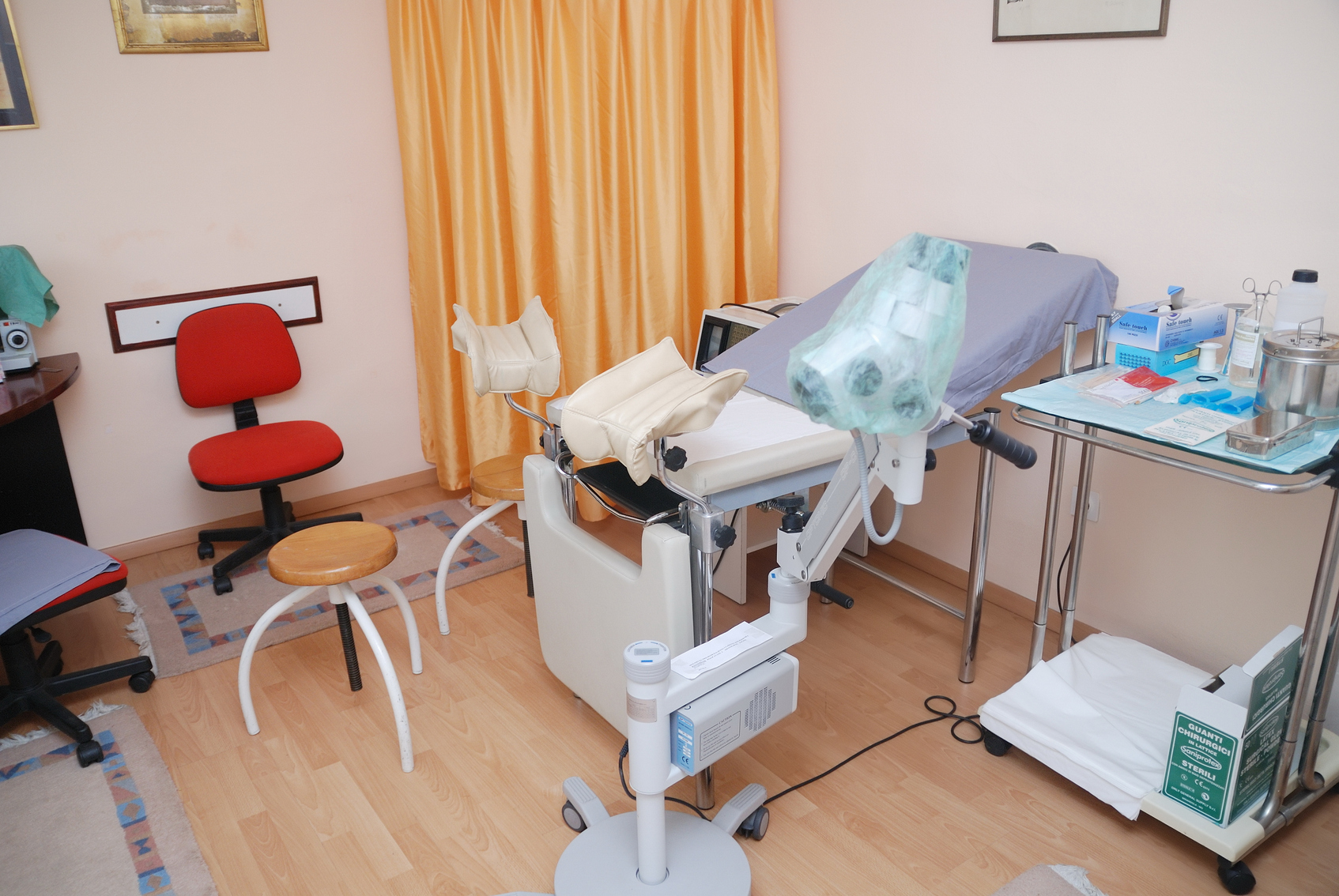
Процедура выполняется в гинекологическом кабинете с помощью стерильных инструментов и включает три основных этапа:
-
Подготовка пациентки. Врач просит женщину занять удобное положение в гинекологическом кресле.
-
Забор материала. С помощью одноразового шпателя или специальной щеточки специалист аккуратно берёт биоматериал со слизистых оболочек половых путей.
-
Затем он наносится на предметное стекло и отправляется в лабораторию.
Как берут анализ из уретры
Процедура может быть немного дискомфортной, но обычно переносится легко. Забор материала производится следующим образом:
-
Врач вводит тонкий аппликатор в уретру на 1–2 см.
-
Деликатными вращательными движениями он собирает биоматериал, который затем наносится на стекло и исследуется в лаборатории.
Это исследование позволяет выявить воспалительный процесс в уретре, а также инфекции, передающиеся половым путём (ИППП).
Как берут мазок из шейки матки
Забор материала из шейки матки — важная часть диагностики инфекций и профилактики онкопатологий. Для этого используют специальную цитощетку, которая позволяет собрать клетки. Процедура проходит так:
-
Мазок берут из влагалища, цервикального канала (шейки матки), уретры (мочеиспускательного канала).
-
Полученный биоматериал наносится на стекло или помещается в транспортную среду.
Эпителий в анализе на флору
Эпителий выстилает слизистую оболочку влагалища, шейки матки и уретры. Его клетки постоянно обновляются, поэтому их присутствие в мазке на флору является нормой. Они выполняют защитную функцию, создавая барьер от инфекций и поддерживая здоровье слизистой оболочки.
-
Норма эпителия в мазке
В норме количество эпителиальных клеток варьируется от 5 до 10 в поле зрения микроскопа. Уровень эпителия может зависеть от менструального цикла, гормонального фона и возраста женщины.
-
Повышенное количество эпителия
Если в мазке обнаруживается избыточное количество эпителиальных клеток, это может указывать на такие воспалительные заболевания, как кольпит, цервицит или уретрит.
-
Отсутствие эпителия
Полное отсутствие эпителиальных клеток встречается реже и зачастую связано с атрофическими изменениями слизистой. Они характерны для периода менопаузы, когда уровень эстрогенов снижается. Это приводит к истончению слизистой и снижению её защитных свойств.
Если результаты анализа показывают отклонения от нормы, необходимо проконсультироваться с врачом. Он определит причину изменений и назначит соответствующее лечение или дополнительные исследования.
Лейкоциты в соскобе на флору
Белые кровяные клетки играют значимую роль в иммунных процессах, защищая организм от инфекций и воспалений.
-
Норма лейкоцитов
В зависимости от того, из какой части половых органов берется мазок, нормальное количество лейкоцитов может немного различаться:
-
Во влагалище - до 10 лейкоцитов в поле зрения.
-
В шейке матки - до 30.
-
В уретре - до 5.
Если эти значения не превышены, это говорит о нормальном состоянии слизистой и отсутствии активных воспалений.
-
Повышенное количество лейкоцитов
Если в мазке обнаруживается значительное увеличение уровня лейкоцитов, это может указывать на наличие воспалительных заболеваний. Например:
-
Вагинит — воспаление слизистой влагалища, часто вызванное инфекцией или нарушением микрофлоры.
-
Эндоцервицит — воспалительное заболевание внутреннего канала шейки матки, которое также может быть связано с инфекциями.
-
Уретрит — воспаление уретры, часто связанное с ИППП.
Увеличение числа белых кровяных клеток также может происходить при травмах слизистой, после полового акта или медицинских процедур.
В любом случае это требует дополнительного обследования для выявления причины. Врач может назначить ПЦР для выявления инфекции, УЗИ мочеполовой системы или бакпосев для уточнения диагноза.
Контроль уровня лейкоцитов помогает своевременно обнаружить воспалительные процессы, что позволяет предотвратить развитие осложнений, таких как хронические инфекции или бесплодие.
Смешанная флора в мазке
Это состояние, при котором в биоматериале одновременно присутствуют как полезные микроорганизмы, так и условно-патогенные. В норме во влагалище преобладают лактобациллы, которые поддерживают нормальный кислотно-щелочной баланс и защищают от инфекций. Однако в случае нарушения микрофлоры могут появляться, например, кокки, грибы (Candida), гарднереллы и другие условно-патогенные бактерии.
Смешанная флора в мазке может возникнуть по разным причинам, среди которых:
-
Нарушение гормонального баланса, например, при приеме оральных контрацептивов, беременности или менопаузе.
-
Прием антибиотиков: убивая как патогенные, так и полезные микроорганизмы, антибактериальные препараты могут приводить к дисбалансу. Особенно часто это происходит при длительном их применении.
-
Наличие бактериальных или грибковых инфекций, в том числе, ИППП (сифилис, гонорея, хламидиоз и трихомониаз).
В случае преобладания условно-патогенных микроорганизмов (кокков, гарднерелл и др.), могут развиться заболевания, такие как:
Бактериальный вагиноз – нарушение нормальной микрофлоры, при котором число лактобацилл значительно снижается, а количество анаэробных бактерий, таких как гарднереллы, увеличивается.
Кандидоз (молочница) – грибковая инфекция, вызванная чрезмерным ростом грибов рода Candida.
При выявлении смешанной флоры важно провести дополнительную диагностику для выявления причины дисбаланса.
Патологические микроорганизмы в анализе на флору
Их выявление требует особого внимания, так как это может свидетельствовать о развитии следующих заболеваний:
-
Гонококки - бактерии, являющиеся возбудителями гонореи. Это ИППП, которое поражает слизистые оболочки половых органов, а также может затронуть глаза, горло и прямую кишку. Симптомы включают болезненные ощущения при мочеиспускании, обильные выделения, боль внизу живота. Если обнаружены гонококки, необходима терапия антибиотиками, чтобы предотвратить осложнения, такие как бесплодие или хронические воспаления.
-
Трихомонады. Это микроорганизмы, вызывающие трихомониаз, одну из самых распространенных ИППП. Трихомониаз может протекать бессимптомно, но часто вызывает зуд, жжение, плохо пахнущие выделения и болезненные ощущения при половом акте. Трихомонады могут также привести к воспалению шейки матки (цервицит) и повышению риска бесплодия. Данное заболевание лечится противомикробными препаратами.
-
Микроскопические грибы, например, рода Candida, являются причиной кандидоза(молочницы). Это грибковая инфекция, которая обычно проявляется в виде творожистых выделений. Кандидоз может возникнуть при снижении иммунитета, после антибиотикотерапии, а также во время беременности или менопаузы из-за гормональных изменений. Терапия обычно включает использование противогрибковых препаратов, как местного, так и системного действия.
-
Кокковая флора — это группа бактерий, в основном состоящая из стрептококков и стафилококков, которая может стать причиной дисбактериоза влагалища. При его развитии очень часто вместо лактобацилл на первый план выходят кокки, что может привести к различным воспалениям (вагинит, цервицит). Для терапии применяют антибиотики, препараты для восстановления микрофлоры, а также корректируют образ жизни.
Выявление патологических микроорганизмов в мазке на флору требует немедленного реагирования и правильного лечения. Несвоевременное лечение может привести к развитию хронических заболеваний, а также негативно сказаться на репродуктивной функции.
Гинекологический мазок — это простой и доступный способ диагностики, который помогает сохранить и укрепить женское здоровье.