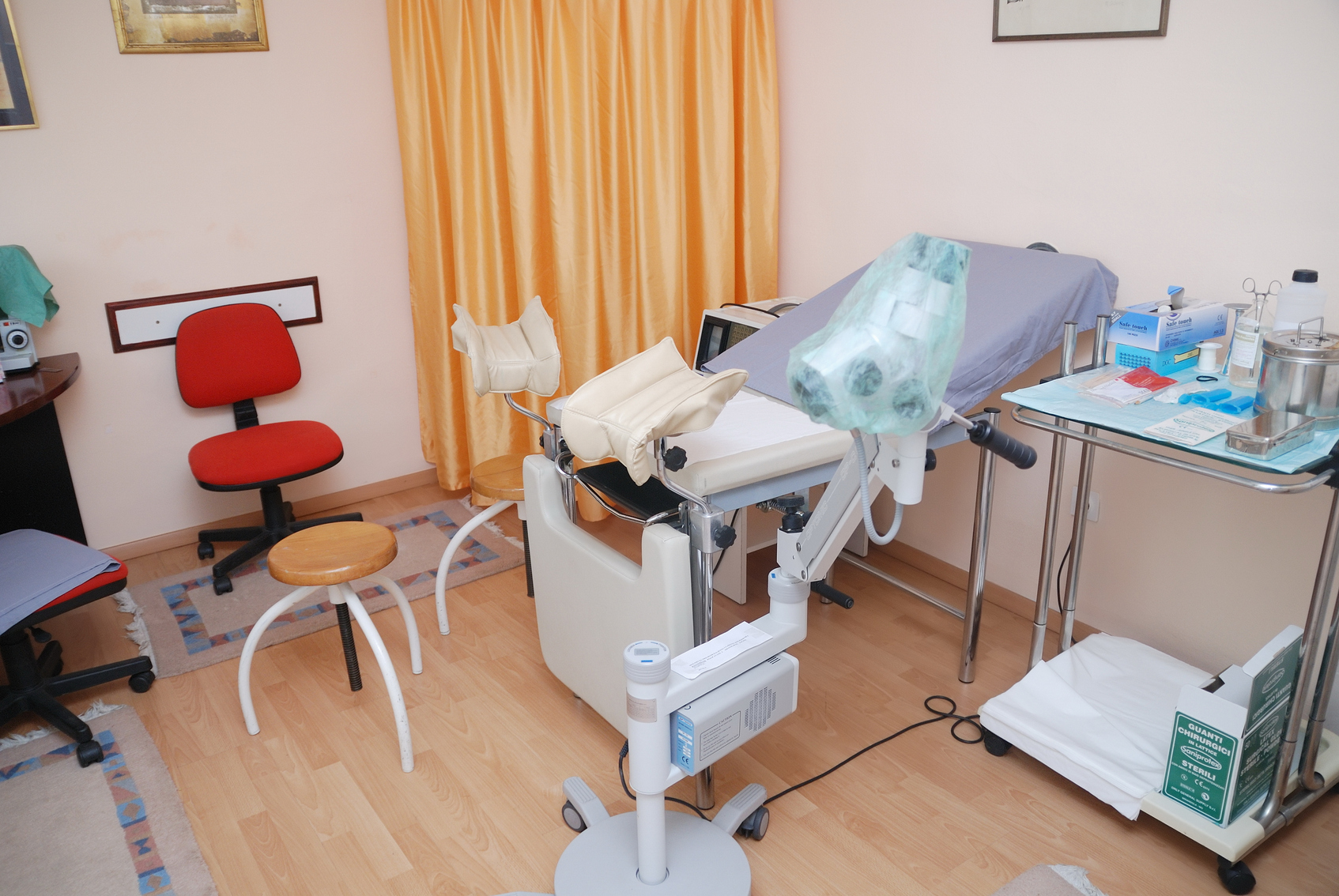
про услугу
Современная гинекология располагает множеством высокоточных методов диагностики, позволяющих выявить заболевания на самых ранних стадиях. Один из них — вульвоскопия. Эта простая и неинвазивная процедура помогает врачу оценить состояние наружных половых органов, вовремя обнаружить воспаления, вирусные поражения, предраковые изменения и новообразования. Вульвоскопия особенно ценна в тех случаях, когда жалобы на дискомфорт есть, а стандартный осмотр не дает полной картины.
В этой статье мы подробно расскажем, что представляет собой вульвоскопия, когда и зачем ее проводят, как к ней подготовиться и чего ожидать от процедуры. Если вы заботитесь о своем здоровье и хотите чувствовать уверенность в завтрашнем дне — эта информация будет полезна.
Что такое вульвоскопия?
Вульвоскопия — это современный и высокоинформативный метод диагностики, который позволяет врачу-гинекологу тщательно исследовать внешние половые органы женщины (вульву), включая преддверие влагалища, большие и малые половые губы, клитор и анальную область. Исследование проводится с применением кольпоскопа — специального оптического прибора, обеспечивающего многократное увеличение и подсветку исследуемой области. Благодаря этому врачу удаётся рассмотреть мельчайшие изменения слизистой оболочки, которые невозможно увидеть при обычном осмотре.
Процедура абсолютно безопасна, не сопровождается нарушением целостности тканей, не требует анестезии и в большинстве случаев переносится комфортно. Вульвоскопия позволяет оценить состояние кожи и слизистых, выявить признаки воспаления, вирусных инфекций (в том числе ВПЧ), предраковых изменений и онкопатологии. Исследование часто сочетается с кольпоскопией — осмотром шейки матки и влагалища — что дает возможность получить комплексную информацию о состоянии нижнего отдела половой системы женщины и при необходимости своевременно принять меры.
Что показывает вульвоскопия?

С помощью вульвоскопии врач получает ценную визуальную информацию, необходимую для точной диагностики заболеваний наружных половых органов. В процессе обследования могут быть выявлены:
- острые или хронические воспалительные изменения, включая вульвит и вульвовагинит;
- вирусные поражения, такие как остроконечные кондиломы, герпетические высыпания, папилломы;
- изменения цвета и структуры слизистой (гиперемия, депигментация, гиперкератоз);
- участки дисплазии и интраэпителиальной неоплазии, указывающие на возможное развитие онкологических процессов;
- новообразования различной природы — от доброкачественных кист до подозрительных узелков;
- рубцовые деформации, последствия травм, разрывов при родах, операций;
- микротрещины, хронические эрозии, плохо заживающие участки;
- признаки кожных заболеваний, таких как склероатрофический лишай;
- лейкоплакия вульвы.
Также в ходе исследования врач может определить необходимость проведения биопсии — забора небольшого участка ткани для лабораторного анализа. Таким образом, вульвоскопия служит важным инструментом для дифференциальной диагностики доброкачественных, предраковых и злокачественных процессов и помогает сформировать индивидуальный план лечения.
Показания к проведению вульвоскопии

Вульвоскопия может назначаться как при наличии выраженных жалоб, так и в рамках расширенного профилактического осмотра, особенно у пациенток из групп риска. К числу основных показаний относятся:
- ощущение зуда, жжения, покалывания или боли в области наружных половых органов;
- выделения с необычным запахом, цветом или консистенцией;
- появление новообразований — папиллом, бородавок, кондилом;
- изменение внешнего вида кожи и слизистой (покраснение, побеление, потемнение, отёчность);
- длительно незаживающие трещины, язвочки, эрозии;
- симптомы, указывающие на возможное инфицирование вирусами, передающимися половым путем (включая ВПЧ и герпес);
- контроль за состоянием тканей после оперативного вмешательства, лазерного лечения, химио- или лучевой терапии;
- уточнение диагноза перед биопсией подозрительных участков;
- наблюдение при подозрении на лейкоплакию, лишай, дисплазию.
Процедура также рекомендована женщинам, имеющим отягощённый онкологический анамнез, носительницам ВПЧ высокого онкогенного риска, а также пациенткам в менопаузе и перименопаузе, когда возрастает вероятность развития фоновых и предраковых состояний. Регулярная вульвоскопия позволяет выявить патологию на самых ранних стадиях и вовремя начать лечение.
Подготовка к процедуре
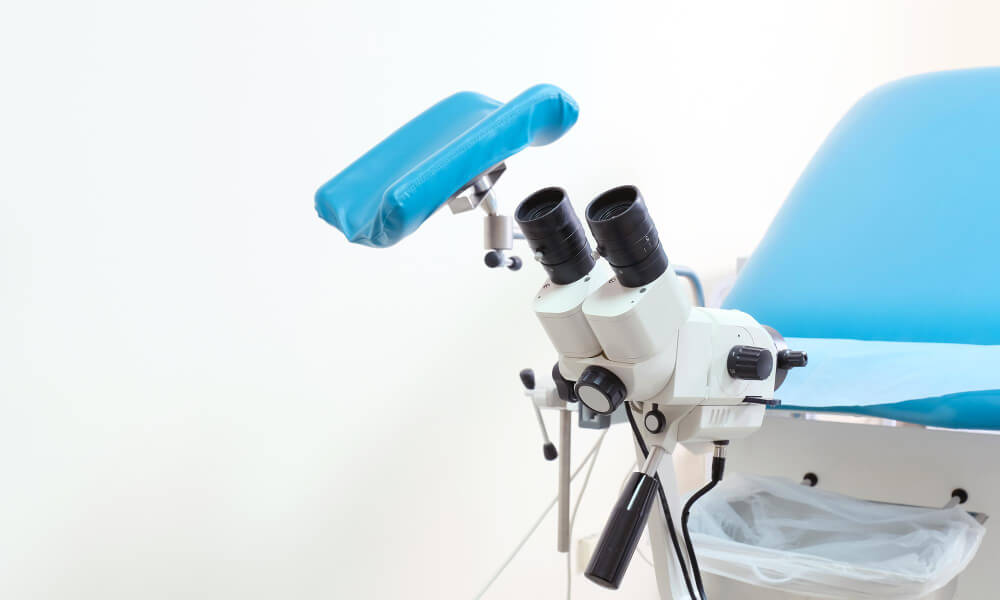
Хотя вульвоскопия не требует особой подготовки, соблюдение ряда рекомендаций поможет врачу получить максимально точную и достоверную картину состояния тканей. Это минимизирует риск искажения результатов и повышает эффективность диагностики.
Перед процедурой желательно:
- воздержаться от половой близости за 24–48 часов — это исключит механическое раздражение слизистой;
- не использовать вагинальные препараты (свечи, кремы, гели, таблетки, спреи) минимум за сутки до исследования, чтобы их остатки не исказили визуальную оценку;
- отказаться от спринцеваний — они нарушают естественную микрофлору и затрудняют диагностику воспалительных процессов;
- не посещать бани, сауны, бассейны за сутки — воздействие высокой температуры и хлорированной воды может изменить состояние слизистой;
- лучше всего проводить исследование в первой фазе менструального цикла — на 5–10 день, сразу после окончания месячных, когда ткани менее отечны и риск воспалений минимален.
Если пациентка уже проходила подобные обследования ранее — кольпоскопию, биопсию, сдачу мазков на онкоцитологию или ПЦР-диагностику, — желательно взять с собой их результаты. Это позволит врачу сопоставить данные, оценить динамику состояния и при необходимости скорректировать дальнейший план обследования и лечения.
Как проходит вульвоскопия?
Процедура проводится в амбулаторных условиях и занимает в среднем от 10 до 20 минут, не требуя госпитализации или наркоза. Она проходит безболезненно для большинства женщин и не вызывает дискомфорта при соблюдении стандартного протокола.
Стандартные этапы обследования выглядят так:
- Пациентка располагается на гинекологическом кресле, как при обычном осмотре.
- Врач выполняет первичный осмотр наружных половых органов при хорошем освещении.
- Кольпоскоп (оптический прибор с подсветкой и увеличением) устанавливается на расстоянии 15–20 см. Он не соприкасается с телом, поэтому не вызывает болевых ощущений.
- При необходимости врач проводит пробу с растворами: наносит 3–5% уксусную кислоту и/или раствор Люголя. Это помогает лучше визуализировать участки, в которых могут происходить предраковые изменения, поскольку патологические клетки реагируют на растворы иначе, чем здоровые.
- При выявлении подозрительных или изменённых зон может быть выполнена прицельная биопсия — забор небольшого фрагмента ткани для последующего гистологического анализа.
Во время процедуры врач может сделать фотофиксацию, чтобы сравнивать динамику в дальнейшем. Большинство женщин переносят исследование легко. Лёгкий дискомфорт возможен лишь при воспалении, повреждениях слизистой или индивидуальной гиперчувствительности.
Реабилитация

Если процедура вульвоскопии проведена без взятия ткани на анализ, никакого восстановления обычно не требуется. Пациентка сразу может вернуться к повседневным делам, работе и физической активности. Однако при выполнении биопсии важно соблюдать щадящий режим и придерживаться рекомендаций врача.
В течение 5–7 дней после биопсии рекомендуется:
- воздерживаться от интимной близости, чтобы не травмировать слизистую и не вызвать кровотечение;
- не использовать влагалищные тампоны — предпочтительны гигиенические прокладки;
- не принимать ванны, не посещать бассейн, баню или сауну — чтобы снизить риск инфицирования;
- избегать активных физических нагрузок, в том числе, занятий спортом и поднятия тяжестей.
После биопсии возможно появление слабых кровянистых выделений, ощущения тянущей боли внизу живота — это нормальная реакция организма. Обычно такие симптомы проходят самостоятельно в течение пары дней. Однако если наблюдается обильное кровотечение, резкие боли, повышение температуры или гнойные выделения — необходимо срочно обратиться к врачу. Эти симптомы могут указывать на осложнение и требуют немедленной медицинской помощи.
Таким образом, реабилитация после вульвоскопии минимальна и зависит от объёма вмешательства. Соблюдение несложных рекомендаций позволяет избежать неприятных последствий и способствует быстрому восстановлению.
Вульвоскопия — это важное обследование, позволяющее своевременно выявить патологические процессы в области вульвы. Процедура проста, не требует сложной подготовки и может проводиться как в рамках планового осмотра, так и по показаниям. При наличии жалоб, новообразований, хронического дискомфорта или для контроля после лечения — не откладывайте визит к гинекологу.
Современные клиники и центры женского здоровья предлагают проведение вульвоскопии с использованием высокоточного оборудования и в комфортных условиях. Своевременное обследование — залог женского здоровья и уверенности в завтрашнем дне.
Вопросы и ответы
Чем отличается вульвоскопия от кольпоскопии?
Вульвоскопия — это визуальный осмотр наружных половых органов (вульвы) с помощью кольпоскопа. Кольпоскопия же направлена на исследование влагалища и шейки матки. Хотя оба метода проводятся одним и тем же прибором, зоны их применения различаются. Часто эти процедуры выполняются в комплексе для получения полной картины состояния женской репродуктивной системы. Совместное проведение позволяет врачу оценить, нет ли патологии сразу на нескольких уровнях: от наружных тканей до шейки матки.
Сколько ждать результаты вульвоскопии?
Если в процессе вульвоскопии не проводилась биопсия, врач может озвучить предварительное заключение уже на приёме. При необходимости забора ткани для гистологии срок ожидания результатов обычно составляет от 5 до 10 рабочих дней. Точное время зависит от лабораторной нагрузки и технических возможностей клиники. Некоторые центры предлагают экспресс-диагностику, но чаще всего окончательное заключение выдается через 1–2 недели.
Больно ли делать биопсию вульвы?
Биопсия — процедура, сопровождающаяся местной анестезией. Врач использует обезболивающий препарат, чтобы минимизировать неприятные ощущения. Большинство женщин описывают её как терпимую, сравнимую с уколом или кратковременным пощипыванием. После процедуры возможен легкий дискомфорт, болезненность или умеренные выделения в течение 1–2 дней. Эти симптомы обычно не требуют специального лечения и проходят самостоятельно. При необходимости можно принять простые обезболивающие, рекомендованные врачом.
Можно ли делать вульвоскопию во время беременности?
Да, вульвоскопия допустима во время беременности и считается безопасной для женщины и будущего ребёнка. Она не вызывает маточных сокращений и не оказывает физического воздействия на плод. Процедура может быть назначена при подозрении на инфекции, новообразования, проявления ВПЧ или при необычных жалобах пациентки.
Если возникает необходимость в биопсии — врач оценивает риски и принимает решение индивидуально. При отсутствии неотложных показаний инвазивные вмешательства стараются отложить до родов, чтобы исключить даже минимальные потенциальные осложнения.
Когда лучше проходить вульвоскопию?
Оптимальное время — 5–10 день менструального цикла, то есть, сразу после окончания месячных. В это время слизистая оболочка наиболее «спокойна»: нет выраженного отека, гиперемии или гормонального воздействия, что позволяет врачу лучше рассмотреть детали.
Однако при наличии острых симптомов — боли, зуда, новообразований, подозрений на инфекции — обследование может быть проведено в любой день, кроме периода активного кровотечения. Главное — соблюдать рекомендации по подготовке и обсудить нюансы с врачом на приеме.